T. 0660 489 4080
M. mail@orthowalther.at
A. Sechskrügelgasse 6 / 2 a&b, 1030 Wien
WAHLARZT – PRIVATE PRACTICE

Dr. Maximilian Walther
Specialist in Orthopaedics and Orthopaedic surgery
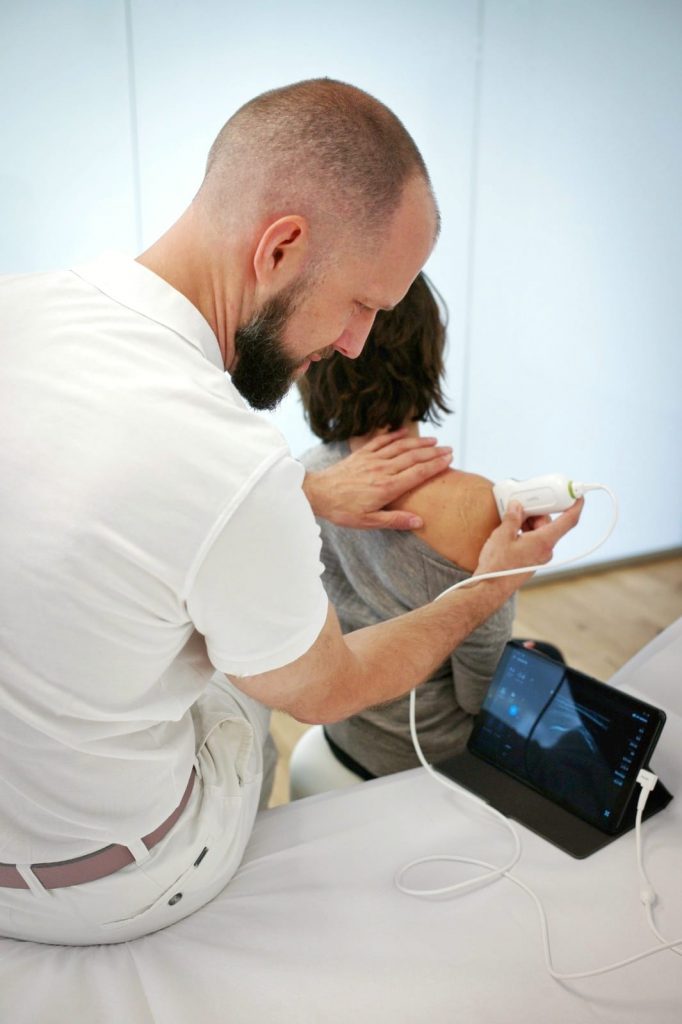
Every treatment begins with a wide-ranging discussion of your symptoms and a full and detailed examination.
True to the principles of evidence-based medicine, at my practice I can give your orthopaedic problems the time they deserve, so that together we may identify a suitable therapy, tailored to your needs.
My extensive education and experience, backed-up by continuous further training, enable me to find the quickest and most effective way to making you feel fit and well again.
If an operation is considered necessary, I personally conduct it with the assistance of our team at the Herz-Jesu Krankenhaus Wien, located at Baumgasse 20A, 1030 Vienna. Here you can enjoy the comfort of highly professional care, provided not only by both myself and the full nursing and medical team of the 2nd orthopaedic department, but also by our well coordinated departments of anaesthesia and internal medicine.
Hip

Changes and wear in the hip joint lead to restricted movement accompanied by pain. At my practice, you will receive a thorough examination in order to establish the primary cause of your problem. Many factors influence the circular movement in the hip, and most problems respond extremely well to conservative treatment. If you suffer from advanced wear in the joint, hip endoprosthesis surgery (implant of a new hip joint), preferably via the anterior approach, offers reliable reduction in pain and the possibility of returning to the vast majority of sporting activities.
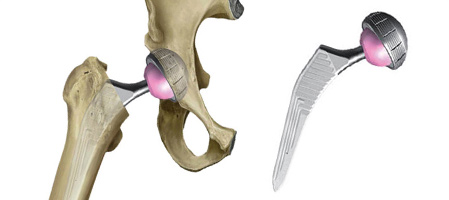
An anterior approach using the AMIS method is my standard approach in this case, as it does not damage muscles or tendons, and the skin incision remains small. Further advantages are a quicker rehabilitation and significantly reduced luxation risk (dislocation). This method should only be performed by surgeons with extensive experience and practice in its application. The type of implants used have proven successful in thousands of patients, and some have even been specifically designed for this particular approach (AMIS). After the operation, you will remain in hospital for between 3 and 5 days. On release you will be able to walk and will be able to go up and down stairs with almost no discomfort.
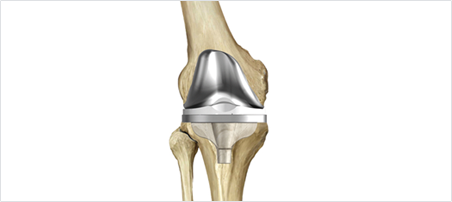
KNEE
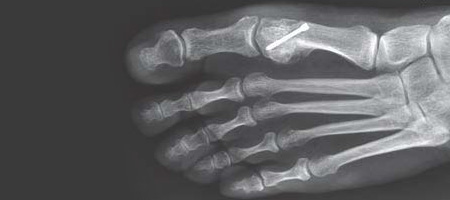
FOOT, ANKLE, JOINT
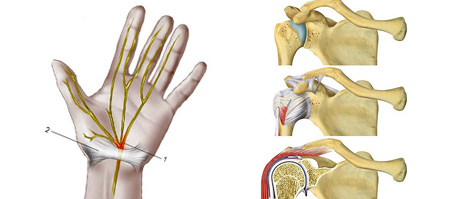
Hand, Ellbogen, Schulter
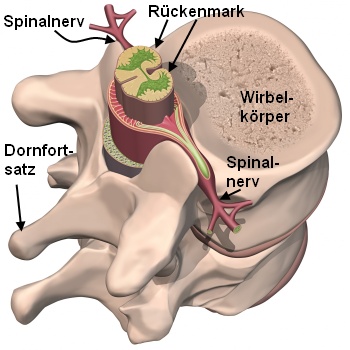
Wirbelsäule
SHOCKWAVE THERAPY
ACP / Autohemotherapy

This therapy brings your very own growth factors to the painful area. After a venous blood drawing, the blood components are separated from each other in the centrifuge, resulting in a platelet concentrate plasma. This plasma is injected in the treated area and increases dramatically cell growth in muscles, tendons and bones.
The applied growth factors help the cellular healing of the bones, cartilages and connective tissue.
There are 4 medical surveys proving the efficacy of the ACP-Therapy in the following indications:
- Minor or moderate arthosis (Level I-III)
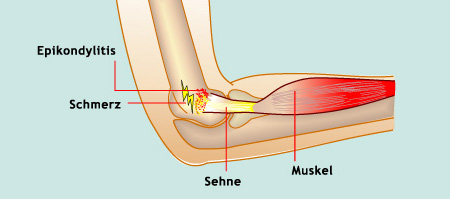
- Epicondylitis
- Plantar fasciitis
- Patellar tendinitis
ACP-Autohemotherapy is a particularly low side effects treatment and is carried out directly in our practice.
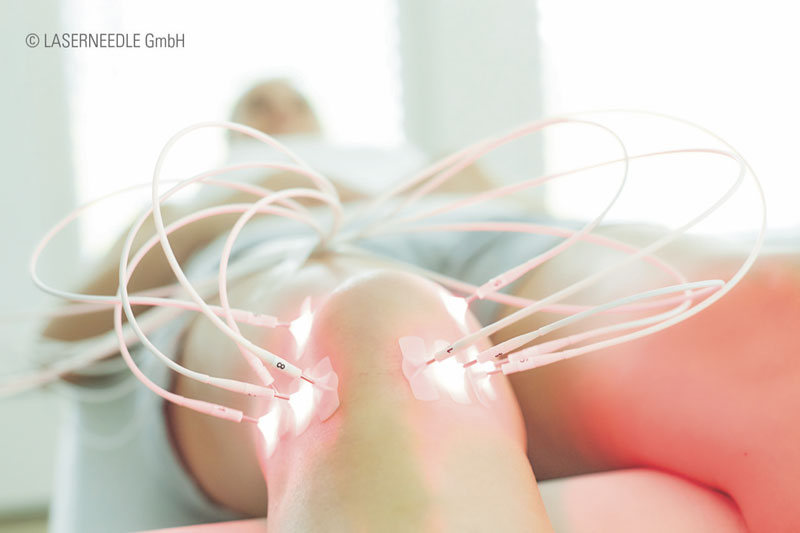
Laserneedle
About me
DR.MED.UNIV. MAXIMILIAN WALTHER
Married, one daughter
Medical studies at the Universities of Vienna and Graz
Training as a specialist in Orthopaedics and Orthopaedic surgery at the BHS Vienna hospital
Study visits and advanced training courses on the subject of hip surgery in France and Switzerland
Implementation of an AMIS hip outpatient clinic
Senior Physician 2. orthopädischen Abteilung Herz-Jesu Krankenhaus Wien
Specialist in hip and knee joint surgery
Certified Senior Surgeon under the EndoCert-Certification system

Contact
Wahlarzt – Private practice
Sechskrügelgasse 6 / 2 a&b, 1030 Vienna
To get to the practice using public transport: Via the underground U3 line: Get off at Rochusgasse, take the lift or stairs to the market, righthand side of the church 50m Busses 4A and 74A, Station Rochusgasse 24 parking possibilty in the same building
T. 0660 489 4080 M. mail@orthowalther.at
Important: Please make sure to duly cancel your appointment if you are not able to keep it. I reserve the right to charge a cancellation fee in the event of an unexcused no show.